Article Text
Statistics from Altmetric.com
- cardiovascular medicine
- interventional cardiology
- ischaemic heart disease
- interventional cardiology
- clinical diagnostic tests
Description
Atheroembolism is a rare but feared complication of arteriography, causing a myriad of signs and symptoms including livedo reticularis, abdominal pain, cyanosis of the toes and renal injury. The main cause is a rupture of atherosclerotic plaque in vessel walls and its embolisation to small diameter vessels affecting more frequently skin and kidneys.1 Here, we present a 69-year-old Hispanic male with medical history of hypertension, type 2 diabetes mellitus and unstable angina status post drug-eluting stent in the left anterior descending coronary artery placement 10 days prior to admission, who arrived to the emergency department with intense diffuse sharp abdominal pain, nausea, vomiting, oliguria and lower extremity pain. Physical examination disclosed livedo reticularis in lower extremities (figure 1), tender abdomen with decreased bowel sounds and funduscopy positive for a Hollenhorst crystal observed in right inferotemporal quadrant (figure 2) and increased creatinine and blood urea nitrogen. Patient was treated with methylprednisolone 125 mg three times a day which improved patient’s abdominal symptoms, renal function and skin findings. He was discharged 16 days later with prednisone 50 mg po and was followed up over a year with resolution of initial symptoms. Management of atheroembolism is usually supportive and depends on the affected organ; to our knowledge, there are no formal studies that have evaluated treating this complication with anti-inflammatory therapies.2 3 Physical exam is fundamental when approaching patient like this, funduscopy was an essential part of the examination and spared the patient from undergoing invasive diagnostic studies like biopsies, as well as opportune initiation of treatment.
Left foot sole with findings consistent with livedo reticularis and blue toe sign.
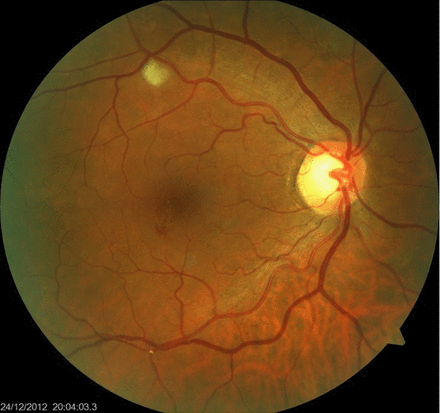
Funduscopy picture where a Hollenhorst crystal can be observed in right inferotemporal quadrant.
Learning points
Funduscopy is an important part of the physical exam and needs to be done in all patients examined.
When examining a patient, we need to take into account multiple differential diagnoses; in this specific case, contrast-induced renal failure could be the cause of the majority of the patient’s symptoms, but after using a combination of physical exam findings and differential diagnosis, adequate treatment was started.
There are diseases that do not always have a set treatment; bibliographic review needs to be made in these cases in order to offer our patient the best change to improve.
Footnotes
Contributors AI was responsible for the patient care, editing of the figures, writing of the manuscript and bibliographic search. OG was responsible for the manuscript editing and details and bibliographic search. AR was repsonsible for the bibliographic search. FL was the senior advisor responsible for patient care, fundoscopy technique and treatment.
Competing interests None declared.
Patient consent Obtained.
Provenance and peer review Not commissioned; externally peer reviewed.