Summary
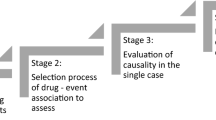
As with any other study method, ‘spontaneous reporting’ in pharmacovigilance is a process of data acquisition, assessment, presentation and interpretation. The provision of information (i.e. of interpreted data) concerning previously unknown, or otherwise important adverse drug reactions is a major goal. The assessment of case reports in spontaneous reporting takes place in 2 steps: first the assessment of each case individually, and secondly the interpretation of the aggregated data. The latter step is only completed for a minority of case reports, such as when actions or measures are deemed necessary.
Uncertainty in case reports regarding the involvement of the suspected drugs is an inherent drawback of spontaneous reporting. Standardised case-causality assessment has become a routine at pharmacovigilance centres around the world. It aims at a decrease in ambiguity of the data and plays a role in data exchange and the prevention of erroneous conclusions. A variety of systems for standardised causality assessment have been developed, ranging from short questionnaires to comprehensive algorithms. Since none of the available assessment systems has been validated (i.e. shown to consistently and reproducibly produce a fair approximation of the truth), causality assessment has only limited scientific value. Causality assessment neither eliminates nor quantifies uncertainty but, at best, categorises it in a semiquantitative way.
Routine causality assessment is usually part of the first step in case assessment, and is based on a general system that is intended for all reactions and all drugs. During the subsequent phase of aggregated assessment, causality assessment is likely to be repeated and the use of a specific aetiological-diagnostic system may be more appropriate. It may be recommended to restrict case-causality assessment to selected case reports that are likely to play an active role in pharmacovigilance and to use specific systems, adapted to the reaction or problem involved.
It is an inherent limitation of spontaneous reporting that, with the exception of rare proof-positive case reports, conclusive evidence cannot usually be produced. Standardised causality assessment has not really changed this situation. As a rule, confirmation of the connection between a drug and an adverse reaction requires further analytical or experimental study.
Similar content being viewed by others
References
Stephens MDB. The detection of new adverse drug reactions. 2nd ed. Basingstoke: The MacMillan Press, 1988
Meyboom RHB, Egberts ACG, Edwards IR, et al. Principles of signal detection in pharmacovigilance. Drug Saf 1997; 16: 355–65
Bégaud B, Evreux JC, Jouglard J, et al. Unexpected or toxic drug reaction assessment (imputation). Actualization of the method used in France. Thérapie 1985; 40: 111–8
Venulet J. Aspects of standardization as applied to the assessment of drug-event associations. Drug Inf J 1984; 18: 199–210
Meyboom RHB, Royer RR. Causality assessment in the European Community. Pharmacoepidemiol Drug Saf 1992; 1: 87–97
Drug safety monitoring: guidelines for setting up and running of a pharmacovigilance centre. Geneva, World Health Organization. In press
Meyboom RHB, Gribnau FWJ, Hekster YA, et al. Characteristics of topics in pharmacovigilance in the Netherlands. Clin Drug Invest 1996; 4: 207–19
Mann RD. Drug safety alerts — a review of ‘Current Problems’. Pharmacoepidemiol Drug Saf 1992; 1: 269–79
International reporting of adverse drug reactions. Final report of CIOMS Working Group I, Geneva, 1990
WHO Collaborating Centre for International Drug Monitoring (Uppsala). Report Type Q No 23, New to the system — documentation grading, 1996, Oct–Dec
International monitoring of adverse reactions to drugs. Adverse reactions terminology. Uppsala: WHO Collaborating Centre for International Drug Monitoring, 1995
Anatomical Therapeutic Chemical (ATC) Classification Index. Oslo: WHO Collaborating Centre for Drug Statistics Methodology, 1994
Biriel C, Edwards IR. Reasons for reporting adverse drug reactions — some thoughts based on an international review. Pharmacoepidemiol Drug Saf 1997; 6: 21–6
Irey N. Tissue reactions to drugs. Am J Pathol 1976; 82: 617–47
Karch F, Lasagna L. Toward the operational identification of adverse drug reactions. Clin Pharmacol Ther 1977; 21: 247–54
Kramer MS, Leventhal JM, Hutchinson TA, et al. An algorithm for the operational assessment of adverse drug reactions. I. Background, description, and instructions for use. JAMA 1979; 242: 623–31
Naranjo C, Busto U, Sellers EM, et al. A method for estimating the probability of adverse drug reactions. Clin Pharm Ther 1981; 30: 239–45
Venulet J, Ciucci AG, Berneker GC. Standardized assessment of drug-adverse reaction associations — rationale and experience. Int J Clin Pharmacol 1980; 18: 381–8
Emanueli A, Sacchetti G. An algorithm for the classification of untoward events in large scale clinical trials. Agents Actions 1980; 7: 318–22
Jones JK. Adverse drug reactions in the community health setting: approaches to recognizing, counseling and reporting. Fam Community Health 1982; 5: 58–67
Venulet J, Berneker GC, Ciucci AG, editors. Assessing causes of adverse drug reactions. London: Academic Press, 1982
Hutchinson TA, Leventhal JM, Kramer MS, et al. An algorithm for the operational assessment of adverse drug reactions. II. Demonstration of reproducibility and validity. JAMA 1979; 242: 633–8
Leventhal JM, Hutchinson TA, Kramer MS, et al. An algorithm for the operational assessment of adverse drug reactions. III. Results of tests among clinicians. JAMA 1979; 242: 1991–4
Hutchinson TA, Lane DA. Assessing methods for causality assessment of suspected adverse drug reactions. J Clin Epidemiol 1989;42:5–16
Venulet J, Ciucci AG, Berneker GC. Updating of a method for causality assessment of adverse drug reactions. Int J Clin Pharmacol 1986; 24: 559–68
Hallas J, Harvald B, Gram LF, et al. Drug related hospital admissions: the role of definitions and intensity of data collection, and the possibility of prevention. J Int Med 1990; 228: 83–90
Lane DA, Kramer MS, Hutchinson TA, et al. The causality assessment of adverse drug reactions using a Bayesian approach. Pharm Med 1987; 2: 265–83
Jones JK. Approaches to evaluating causation of suspected drug reactions. In: Strom BL, Velo G, editors. Drug epidemiology and post-marketing surveillance. New York; Plenum Press, 1992: 103–13
Kramer MS. Clinical epidemiology and biostatistics. Berlin: Springer Verlag, 1988
Lanctôt KL, Naranjo CA. Computer-assisted evaluation of adverse events using a Bayesian approach. J Clin Pharmacol 1994; 34: 142–7
Lubsen J. Essentials of Bayesian diagnostic reasoning. Neth J Med 1995; 47: 252–9
Girard M. Testing the methods of assessment for adverse drug reactions. Adv Drug React Ac Pois Rev 1984; 4: 237–44
Pere JC, Bégaud B, Haramburu F, et al. Computerized comparison of six adverse drug reaction assessment procedures. Clin Pharmacol Ther 1986; 40: 451–61
Bénichou C, editor. Adverse drug reactions. A practical guide to diagnosis and management. Chichester: John Wiley & Sons, 1994
Stratton KR, Howe CJ, Johnston RB, editors. Adverse events associated with childhood vaccines. Evidence bearing on causality. Washington, DC: National Academy Press, 1994
Olsson S, editor. National pharmacovigilance systems. Country profiles and overview. Uppsala: The Uppsala Monitoring Centre, 1997
Meyboom RHB. The Netherlands. In: Inman WHW, Gill EP, editors. Monitoring for drug safety. Lancaster: MTP Press, 1986: 107–17
Johnson JM. Reasonable possibility: causality and postmarketing surveillance. Drug Inf J 1992; 26: 553–8
Edwards IR, Biriell C. Harmonisation in pharmacovigilance. Drug Saf 1994; 10:93–102
Castle W. Adverse drug reactions: scope and limitations of causality assessment and the use of algorithms. Int J Risk Safety Med 1991; 2: 185–92
Hutchinson TA, Flegel KM, Ho Pingkong H, et al. Reasons for disagreement in the standardized assessment of suspected adverse drug reactions. Clin Pharmacol Ther 1983; 34: 421–6
Bégaud B, Boisseau A, Albin H, et al. Comparaison de quatre méthodes d’imputabilité des effects indésirable médica-menteux. Thérapie 1981; 36: 65–70
Lagier G, Vincens M, Lefebvre B, et al. Imputation médicament par médicament en pharmacovigilance. Essai de comparaison de différentes méthodes. Thérapie 1983; 38: 295–302
Leroy O, Bégaud B, Dangoumau J, et al. Etude comparative de quatre méthodes d’imputabilité. Thérapie 1981; 36: 223–7
Busto U, Naranjo CA, Sellers EM. Comparison of two recently published algorithms for assessing the probability of adverse drug reactions. Br J Clin Pharmacol 1982; 13: 223–7
Louik C, Lacouture PG, Mitchell AA, et al. A study of adverse reaction algorithms in a drug surveillance program. Clin Pharmacol Ther 1985; 183–7
Blanc S, Leuenberger P, Berger JP, et al. Judgements of trained observers on adverse drug reactions. Clin Pharm Ther 1979; 25: 493–8
Frick PA, Cohen LG, Rovers JP. Algorithms used in adverse drug event reports: a comparative study. Ann Pharmacother 1997; 31: 164–7
Lanctôt KL, Naranjo CA. Comparison of the Bayesian approach and a simple algorithm for assessment of adverse drug events. Clin Pharmacol Ther 1995; 58: 692–8
Auriche M, Loupi E. Does proof of causality ever exist in pharmacovigilance? Drug Saf 1993; 9: 230–5
Guidelines for good clinical practice (GCP) for trials on pharmaceutical products. WHO Technical Report Series, No. 850. Geneva: World Health Organization, 1995
Hoskins RE, Mannino S. Causality assessment of adverse drug reactions using decision support and informatics tools. Pharmacoepidemiol Drug Saf 1992; 1: 235–50
Edwards IR, Lindquist M, Wiholm BE, et al. Quality criteria for early signals of possible adverse drug reactions. Lancet 1990; 336: 156–8
Harmonizing the use of adverse reaction terms. Definitions of terms and minimum requirements for their use: respiratory disorders and skin disorders [special communication]. Phar-macoepidemiol Drug Saf 1997; 6: 115–27
Meyboom RHB. Good practice in the postmarketing surveillance of medicines. Pharmacy World Sci. Pharm World Sci 1997; 19: 186–90
Stricker BHC, Blok APR, Claas FHJ, et al. Hepatic injury associated with the use of nitrofurans: a clinicopathological study of 52 reported cases. Hepatology 1988; 8: 559–606
Stricker, BHC, Blok APR, Bronkhorst FB, et al. Ketoconazole-associated hepatic injury. J Hepatol 1986; 3: 399–406
Lake-Bakaar G, Scheuer PJ, Sherlock S. Hepatic reactions associated with ketoconazole in the United Kingdom. BMJ 1987;294:419–22
Salama A, Mueller-Eckhardt C. The role of metabolite-specific antibodies in nomifensine-dependent immune hemolytic anemia. N Engl J Med 1985; 313: 469–74
Edwards IR. International drug monitoring. In: Aronson JK, Van Boxtel CJ. Side effects of drugs annual. Vol 19. Amsterdam: Elsevier Science Publishers, 1995: 450–5
Jones JK. Causality assessment of suspected adverse drug reactions, a transatlantic view. Pharmacoepidemiol Drug Saf 1992; 1:251–60
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Meyboom, R.H.B., Hekster, Y.A., Egberts, A.C.G. et al. Causal or Casual?. Drug-Safety 17, 374–389 (1997). https://doi.org/10.2165/00002018-199717060-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/00002018-199717060-00004