Article Text
Statistics from Altmetric.com
Description
Oesophageal varices commonly develop in the setting of portal hypertension. A Sengstaken-Blakemore (SB) tube is sometimes emergently required to control oesophageal bleeding.1 ,2
The normal portal pressure varies from 5 to 10 mm Hg. Portal hypertension occurs when the portal pressure rises above 10 mm Hg. Pressures can rise up to 30 mm Hg, so the pressure exerted and maintained on the oesophageal balloon to tamponade the varices will need to be above 30 mm Hg.
The current practice is to attach a 1 L bag of saline to the tube to maintain traction. However, there are risks associated with this method of traction. These risks include pharyngeal ulcers and mouth ulcers from the local pressure effect. We describe an alternative method of maintaining traction on the SB tube.
We describe the practice of securing the tube with a pair of wooden tongue depressors and padding as shown in figure 1. This has been used by the lead author for 25 years with no adverse events. The patient population includes patients with oesophageal varices. The patients ranged from 18 to 85 years of age. Over 50 patients have been treated by the lead author using this method.
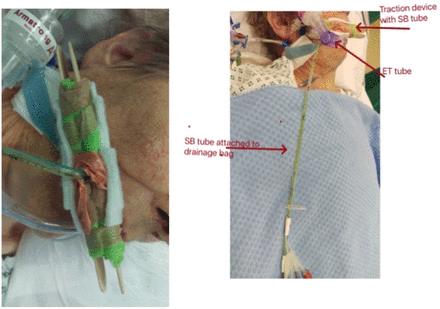
Traction device in use on a patient.
This is an alternative safe method of applying traction without the adverse local pressure effects.
Equipment needed
Equipment needed are McGill forceps, lubrication jelly, 2×60 cc syringes with a luer lock, one large bladder irrigation syringe, a sphygmomanometer or any other hand-held device for measuring pressure, and contrast with water for insertion into the gastric balloon.
Insertion
These patients are usually intubated as the risk of airway contamination is extremely high if balloon tamponade is required to control bleeding. If possible, these cases should be performed in theatre.
Check and confirm there are no air leaks in the gastric and oesophageal balloons.
The tube has markings on it; make sure that these markings are visible when inserting the tube. When it is being inserted endoscopically, direct visualisation of the gastro-oesophageal junction is possible.
Insert a mix of contrast dye and water into the gastric balloon. This will enable visualisation on the subsequent chest X-ray to confirm position postprocedure. Once 150–200 mL of water/contrast mix should have been filled; close the aspiration port.
Pull the balloon until it rests firmly against the gastro-oesophageal junction. An assistant is necessary to maintain this traction until the definitive traction has been set up.
Insert air into the oesophageal balloon. The author prefers to aim for a pressure of 28–30 mm Hg. The normal portal pressure is 5–10 mm Hg and the consequences of pressure necrosis in the oesophagus are serious. The oesophageal balloon is routinely inflated in all patients for a minimum of 4 hours and then the situation is re-evaluated. The oesophageal balloon is deflated at the 4 hour mark and then can be reinflated if necessary. The traction device has been attached with the oesophageal and gastric balloon inflated.
Maintain traction
Various methods of maintaining traction have been described in the literature to date. Some of the more common methods include attaching a 500–1000 mL bag of saline to the SB tube. Other options occasionally favoured in the USA include securing the SB tube to the rim of a helmet.3 However, several users have described this as cumbersome in terms of nursing care. Other institutions have described a method of splitting a tennis ball in half to maintain traction and fix it to the patients face. However, this has the disadvantage of a pressure effect on the patient's teeth and lips. Tennis balls are not readily available to most institutions in an emergent situation. Record the marking at the teeth. Documentation will ensure the tube does not slip and that traction is maintained.
Set up of alternative device
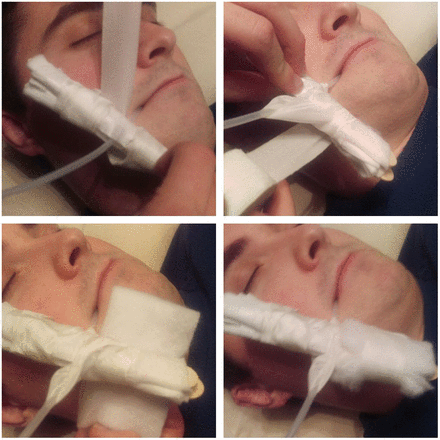
Step 1: Secure a thin rolled up 10×10 cm gauze to the longitudinal surface of each tongue depressor. A sleek tape may be used to secure the gauze (figure 2).
Demonstration of adhesive tape around the tongue depressors.
Step 2: Wrap the tape around the cranial end of the SB tube using two twists, do not cut it from the roll. The SB tube should be cleaned with a swab prior to ensure it is dry before (figure 3).
Demonstration of adhesive tape attachment to the Sengstaken-Blakemore tube.
Step 3: Wrap the sleek tape around both sides of the tongue depressor construct and then finish by wrapping a layer circumferentially around the SB tube (figure 3).
Step 4: Apply a foam wrap to the surface which is in contact with the mouth and lips. We use the same foam that is used in casts as this has been designed to withstand considerable friction (figure 4).
Demonstration of the Sengstaken-Blakemore tube with foam.
Step 5: Take note of the marking and educate staff on the construct. This may be repositioned by the nursing staff by twisting/altering the direction.
Aftercare
Regular suctioning of the oesophageal and gastric lumen is necessary.
Frequent oropharyngeal suctioning is necessary.
Antibiotic prophylaxis and 48 hours of terlipressin are required.
Repeat endoscopy at 24 hours is advised.
In our unit, the oesophageal balloon is deflated at 6–12 hours postinflation.
Repeat endoscopy should be carried out if possible in theatre. These patients are usually intubated.
Potential limitations of using this method could include unfamiliarity with the device. However, this would be overcome by education.
Learning points
The combination of this traction method and ensuring a relatively low pressure is maintained in the oesophageal balloon has resulted in few/no pressure-related complications.
There has been a positive experience with this method. It is cost-effective, easy to assemble and does not have the same rate of pressure-related ulcers as reported in the literature with the saline bag.
There has been a lack of trials or studies reporting on the differing traction methods in securing the Sengstaken-Blakemore (SB) tube. Limitations could include a lack of a standardised method to secure the SB tube.
Footnotes
Contributors EPM used the device. SMOB proof read the manuscript and performed literature review. MR devised the device and proof read the manuscript.
Competing interests None declared.
Patient consent Obtained.
Provenance and peer review Not commissioned; externally peer reviewed.