Article Text
Statistics from Altmetric.com
Description
Trans-septal puncture is a routine approach in most electrophysiology laboratories since atrial fibrillation (AF) and ventricular tachycardia (VT) ablation became common. Here, we report a procedural complication and its safe resolution.
A 68-year-old man was brought in and admitted urgently in our department after sudden onset of palpitations. His medical history included coronary artery bypass graft (CABG), bundle branch block, AF, implanted implantable cardioverter defibrillator (ICD) and episodes of recurrent VT documented after electrophysiological study. From his ICD log it was obvious that he suffered a self-terminated episode of VT. On admission he was haemodynamically stable with a systolic pressure of 110 mm Hg, and had elevated international normalized ratio (INR) (3.1) due to warfarin therapy for his AF. To counter this, 3000 units of human prothrombin complex and 5 mg vitamin K were instituted intravenously and the INR was reduced to 1.2.
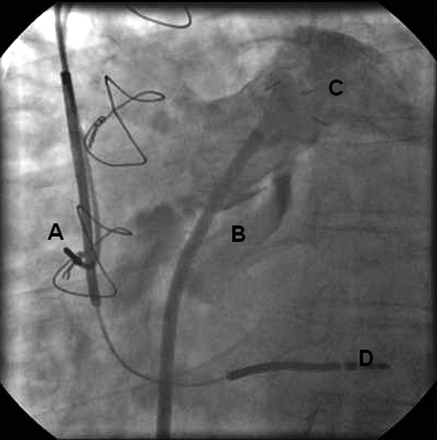
The technique described by Linker and Fitzpatrick1 was used. In the cardiac interventional laboratory under fluoroscopic guidance, contrast was injected to confirm the position of the fossa ovalis and the intra-atrial septum was punctured. However, on advancing the sheath it became evident that it had punctured the left atrial roof and entered the right pulmonary artery (RPA). Figure 1 demonstrates the left anterior oblique view of the RPA with contrast in situ.
Fluoroscopic left anterior oblique view of the right pulmonary artery with contrast in situ. A, right atrium with atrial lead in situ in right atrial appendage; B, left atrium, lying beneath the main pulmonary trunk; C, the main pulmonary artery trunk; D, right ventricular apex with ICD lead in situ.
The procedure was stopped due to this complication. A stiff guide wire was passed across the puncture site prophylactically to counter any untoward bleeding. A decision was taken to transfer the patient to the operation theatre to withdraw the sheath in a controlled environment. Under general anaesthesia and invasive monitoring a transesophageal echocardiography (TOE) probe was inserted to evaluate cardiac anatomy, to assess flow across the perforation and to detect possible pericardial effusion. The ablation sheath was withdrawn under direct TOE imaging (figure 2). The procedure was carried out in the presence of a cardiothoracic surgeon and a perfusionist ready to proceed with opening the chest in the case of massive pericardial effusion. The sheath removal was uneventful. The result of follow-up of this connection was healing with no sequelae.
Transesophageal echocardiography image of the ablation catheter sheath (c) across the interatrial septum. LA, left atrium; RA, right atrium.
Learning point
TOE has become the gold standard modality to monitor several non-coronary interventional procedures owing to its versatility in real-time visualisation of cardiac structures, catheters and devices.2
Footnotes
Competing interests None.
Patient consent Obtained.