Article Text
Statistics from Altmetric.com
Description
A 31-year-old woman experienced sudden onset parieto-occipital headache 2 days postpartum. This resolved spontaneously but recurred at 6 days postpartum, when she reported the worst occipital headache she had ever experienced. Neurological examination was unremarkable. A non-contrast CT scan of the brain revealed subarachnoid haemorrhage (SAH) predominantly distributed in a superficial cortical pattern (figure 1). The patient was urgently transferred to a neurosurgical unit and underwent cerebral digital subtraction angiogram which demonstrated multiple areas of arterial stenosis and dilatation, suggestive of diffuse vasospasm (figure 2). Blood tests for vasculitis and autoimmune disease, urine toxicology screen and cerebrospinal fluid analysis were normal.
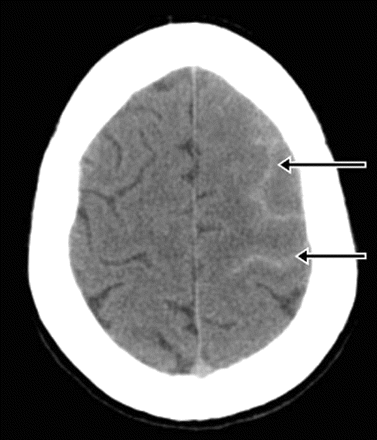
Non-contrast CT scan of the brain taken at initial presentation demonstrating convexity subarachnoid haemorrhage over the cortical surface as opposed to the more common patterns of blood seen after aneurysmal bleeds.
Digital subtraction angiography – left internal carotid injection showing the characteristic findings of dilated and constricted arteries due to vasospasm, grossly and inset in more detail.
Reversible cerebral vasoconstriction syndrome is chracterised by sudden severe headache with cerebral arterial vasoconstriction which spontaneously resolves. It is more prevalent in females and around two thirds of cases are secondary to pregnancy or vasoactive substances including cannabis, cocaine, esctasy, amphetamines and binge drinking. Patients are said to complain of an intense sudden onset headache which may relapse and remit as here. Neurological deficits and seizures may occur at presentation. A quarter to a third will have raised blood pressure during the episode.
Investigations are often directed to excluding aneurysmal subarachnoid bleed and non-contrast CT may show SAH in 20%, usually cortical. Infarction and intracerebral haemorrhage are less common at around 5%.1 Angiogram is definitive with the so-called ‘string of beads’ finding of segmenetal narrowing and dilatation as illustrated here. Nimodipine (60 mg six times daily), which was given here, is said to speed resolution, though more recently aggressive endovascular interventional techniques such as intra-arterial vasodilators and angioplasty have been employed.2
References
Footnotes
-
Competing interests None.
-
Patient consent Obtained.